Last month, a 47-year-old founder came into my office convinced he was healthy. His weight was "normal" — 185 pounds at 5'11", a BMI of 25.8. His primary care doctor had given him a clean bill of health three years in a row. No red flags. No concerns.
His DEXA scan showed 31% body fat and visceral adipose tissue area at nearly double the cardiovascular risk threshold. His appendicular lean mass index was in the lowest quartile for men his age — subclinical sarcopenia that a bathroom scale would never reveal in a hundred years of weighing him.
His scale had been lying to him for years. BMI had done the same. And he wasn't an outlier.
What Is a DEXA Scan, and Why Does It Measure Body Composition Better Than Anything Else?
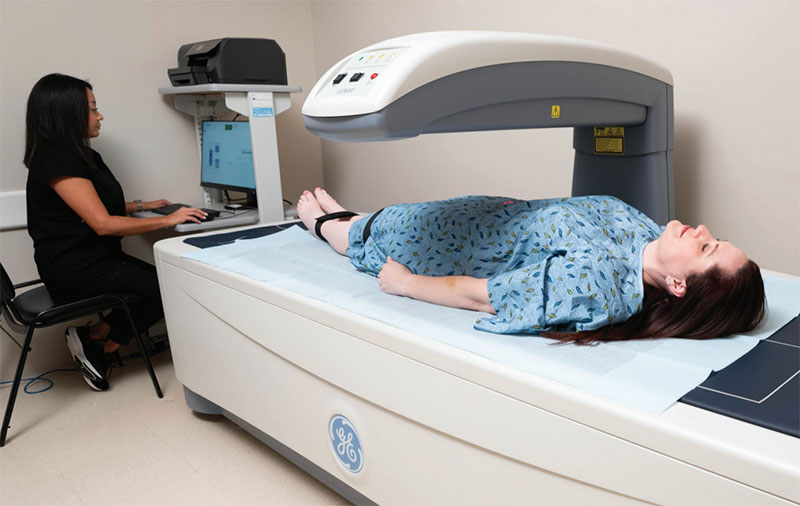
Dual-energy X-ray absorptiometry — DEXA — was originally developed to measure bone mineral density. But the same technology that reads your bone density also provides a precise, three-compartment body composition analysis in about ten minutes. Standard bathroom scales measure gravitational force. They cannot tell fat from muscle, water from inflammation, or a healthy 200-pound athlete from a sarcopenic 200-pound man losing a pound of muscle each year.
DEXA measures your body the way medicine needs to measure it:
Visceral Adipose Tissue
The metabolically dangerous fat packed around your organs — measured independently from subcutaneous fat. This is the number that predicts cardiovascular disease risk, insulin resistance, and systemic inflammation.
Appendicular Lean Mass
The total lean mass in your arms and legs — your functional muscle reserve. Normalized to BMI (ALM/BMI ratio), it is the primary validated clinical marker for sarcopenia screening.
Bone Mineral Density
T-scores and Z-scores at the hip and lumbar spine, simultaneously assessed — the clinical standard for osteoporosis and fracture risk stratification.
DEXA also gives you regional fat distribution — Android vs. gynoid fat patterns and trunk-to-limb ratios — that body fat percentage measurements cannot provide. Two people with identical body fat percentages can have completely different metabolic risk profiles depending on where that fat lives.
Why It Matters: The Science Behind Body Composition
The BMI Problem
Body mass index was developed in the 1830s by a Belgian mathematician named Adolphe Quetelet. He was studying population statistics — not individual health. He never intended it to be a clinical tool for individual patients. And yet here we are, in 2026, still using a 200-year-old population statistic to make individual clinical decisions.
A landmark 2023 cross-sectional study published in the Journal of Family & Community Medicine evaluated 319 adults who underwent whole-body DEXA scans and compared findings to BMI classification. BMI classified 51% of the cohort as obese. DEXA found 92% had excess body fat. Forty percent of participants who BMI classified as "normal weight" were found to be obese or overfat by DEXA — a pattern researchers called "normal-weight obesity."
The same thing happens in reverse. I have patients with BMIs of 28 who are athletes — high muscle mass, low visceral fat, metabolically excellent. BMI calls them "overweight." DEXA tells the truth.
The Visceral Fat Danger
Visceral fat is not passive. It is metabolically active tissue that secretes inflammatory cytokines, disrupts insulin signaling, and contributes to dyslipidemia, insulin resistance, and cardiovascular risk in ways that subcutaneous fat does not. A 2025 meta-analysis found that high visceral adiposity index was associated with a 55% increased risk of cardiovascular disease (RR = 1.55), with each 0.5-unit rise in the visceral adiposity index boosting CVD risk by an additional 19%.
"Two people with identical waist measurements can have vastly different visceral fat. The only way to measure it precisely is imaging. DEXA is that imaging."
Waist circumference gives a rough proxy for abdominal adiposity, but two people with identical waist measurements can have completely different VAT. Subcutaneous fat — the fat under the skin — doesn't carry the same metabolic burden. Only DEXA separates them.
The Sarcopenia Problem Nobody Talks About
The second thing DEXA reveals that scales hide: muscle loss. Sarcopenia — the progressive loss of skeletal muscle mass and strength — begins subtly in your 30s, accelerates after 40, and carries significant mortality risk that most primary care physicians are not screening for.
A 2025 retrospective cohort study published in the Journal of Clinical Medicine followed adults with cardiovascular disease who underwent DEXA body composition analysis. Sarcopenia was present in 37.2% of the cohort. Patients who had both high visceral fat and sarcopenia had 6.74 times the mortality risk of patients with neither condition. And most of those patients had normal BMI.
The ALM/BMI ratio is a practical clinical tool validated to predict adverse outcomes. A 2025 Nature Scientific Reports analysis of patients with type 2 diabetes demonstrated that both ALM/BMI and ALM/height² were significantly associated with insulin resistance, cardiovascular risk markers, and all-cause mortality — independent of total body fat percentage.
The Obesity Paradox, Resolved
You may have heard of the "obesity paradox" — the counterintuitive finding that some individuals with higher BMI appear to have lower mortality in certain studies. DEXA largely resolves this: the paradox appears to be driven by sarcopenic individuals who are "normal weight" by BMI but metabolically impaired — and high-BMI individuals who have high muscle mass, low visceral fat, and excellent metabolic function. BMI conflates them. DEXA distinguishes them.
The Gap in Standard Care
Here is what conventional medicine gives you: weight, height, BMI, and perhaps a waist circumference. These are 20th-century tools applied to 21st-century metabolic disease. They are cheap, fast, and they miss the picture.
Your primary care doctor likely has no DEXA scanner in the office. The test is often reserved for osteoporosis screening in postmenopausal women or older men — never as a routine metabolic assessment for a 45-year-old male executive whose fasting glucose is 96 and who "looks fine." The result is that visceral fat accumulates silently for decades. Muscle mass erodes quietly. And your annual physical tells you your BMI is 26.4 — perfectly normal — while your metabolic risk profile tells a different story.
In my practice, I see this routinely: the lean-looking patient with high visceral fat and early insulin resistance. The patient who gained 20 pounds of muscle and lost 15 pounds of fat but whose scale hasn't moved. The 52-year-old CEO whose annual physical cleared him three years in a row — until his DEXA showed VAT at 178 cm², fasting insulin at 18 μIU/mL, and ALM/BMI in the lowest quartile for men his age. We had a diagnosis the scale could never have given us. We had a target. And we could measure progress.
How We Use DEXA at Pravida Health
Every Foundation membership includes a baseline DEXA scan. We use it not as a one-time snapshot but as a recurring reference — typically every 6 to 12 months — that allows us to track body composition changes with the precision that interventions require.
Specifically, we assess:
- VAT area (cm²) — our primary visceral fat metric, with clear intervention thresholds (low: <100 cm²; moderate: 100–160 cm²; high: >160 cm²)
- ALM/BMI — screened against age- and sex-specific normative data for sarcopenia classification
- Trunk-to-limb fat ratio — an Android distribution marker independent of total body fat percentage
- Bone mineral density — T-scores and Z-scores at the hip and lumbar spine
- Lean mass trajectory — tracked over time to detect early sarcopenia and validate resistance training response
This data doesn't exist in isolation. We integrate it with your fasting insulin and HOMA-IR, your inflammatory markers, your hormone panel, and your VO2 max — because body composition is a symptom of metabolic function, not an independent variable. When I see high visceral fat alongside elevated fasting insulin and low free testosterone in a 48-year-old patient, that's a pattern requiring coordinated intervention — not just "eat less and exercise more."
DEXA makes the invisible visible. And once you can see it, you can measure it. And once you can measure it, you can change it.
What You Can Do Today
1. Stop tracking weight as your primary health metric. The scale is useful for broad trend tracking over weeks, but a 5-pound weight gain during a period of resistance training may represent improved lean mass, not metabolic decline. Weight alone is not a biomarker.
2. Measure your waist circumference. While imperfect, waist circumference above 40 inches in men and 35 inches in women is a validated marker of elevated cardiovascular risk. It costs nothing and takes 30 seconds.
3. Incorporate resistance training now. Muscle is the organ of longevity. Regardless of your body fat percentage, two to three sessions per week of progressive resistance training directly protects your ALM/BMI trajectory and reduces sarcopenia risk.
4. Request a DEXA scan. If your physician doesn't offer one, ask where to get a clinical body composition DEXA in your area. At Pravida Health, it's included in our Foundation membership — baseline, repeat, and integrated with your full metabolic assessment.
Frequently Asked Questions
What is a DEXA scan body composition test?
A DEXA (dual-energy X-ray absorptiometry) body composition scan uses two low-dose X-ray beams to measure fat mass, lean mass (muscle), and bone mineral density across the entire body and in specific regions (trunk, arms, legs). It takes approximately 10 minutes and delivers less radiation than a day of normal background environmental exposure.
How is DEXA different from a body fat percentage on a scale?
Consumer scales and gym bioimpedance devices estimate body composition using electrical resistance, which is highly sensitive to hydration status and varies by device quality. DEXA is a medical imaging modality that directly measures tissue compartments — providing visceral fat area in cm², appendicular lean mass, regional fat distribution, and bone mineral density, none of which bioimpedance can reliably measure.
What is a healthy visceral fat level on a DEXA scan?
DEXA-measured visceral adipose tissue (VAT) area below 100 cm² is generally considered low risk. Between 100 and 160 cm² represents moderate risk; above 160 cm² is associated with significantly elevated metabolic and cardiovascular risk. Two people with identical waist measurements can have vastly different VAT — only DEXA quantifies this directly.
Is a DEXA scan safe?
Yes. A whole-body DEXA scan delivers approximately 1–10 microsieverts of radiation — less than a day of background environmental exposure. A chest X-ray delivers roughly 100 microsieverts; a cross-country flight delivers 20–40 microsieverts. DEXA is safe for annual or semi-annual body composition monitoring.
How often should I get a DEXA scan?
For body composition tracking, every 6 to 12 months is appropriate — long enough to detect meaningful change without over-testing. At Pravida Health, Foundation membership includes a baseline DEXA scan with repeat assessment every 6–12 months as part of ongoing metabolic monitoring.
Can DEXA detect sarcopenia?
Yes. DEXA measures appendicular lean mass (ALM) and calculates ALM/BMI ratio — the primary validated clinical marker for sarcopenia screening. A 2025 study found sarcopenia present in 37% of cardiovascular disease patients, with patients having both high visceral fat and sarcopenia facing 6.74 times the mortality risk of those with neither condition.
Is DEXA included in Pravida Health memberships?
Yes. Every Foundation membership at Pravida Health includes a baseline DEXA body composition scan. Results are integrated with your biomarker panel, hormone assessment, and VO2 max data to build a complete metabolic picture — not treated as an isolated data point.
See What Your Scale Has Been Hiding
Foundation membership at Pravida Health includes baseline DEXA body composition analysis alongside comprehensive biomarkers, hormone assessment, VO2 max testing, and a full metabolic review — all integrated into a personalized longevity plan.
Schedule a Consultation View Memberships